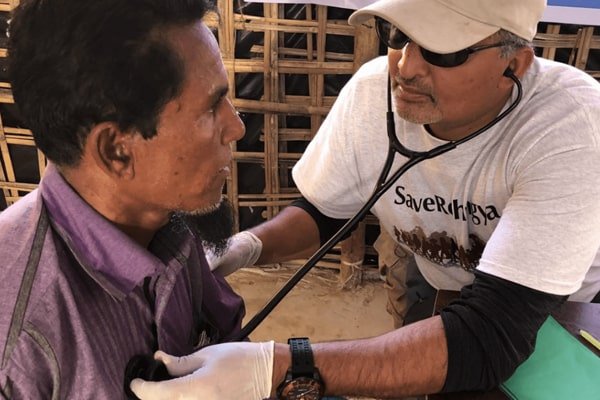
The COVID-19 pandemic has weighed heavily on all countries, overwhelming healthcare systems, shattering economies, and disproportionately affecting vulnerable people such as refugees, asylum seekers, and those living in poverty. In many countries, refugees living in densely populated camps, shelters, or sites were blamed for the spread of SARS-CoV-2. Pre-existing inequalities have deepened, and anti-refugee sentiments have increased.
Social, infrastructural, economic, and health factors have made refugees more vulnerable than others to contracting COVID-19; yet, they are more likely to be left out of the pandemic response measures. Listed below is an explanation of the countless inequalities that refugees have faced since the pandemic began.
Refugees are often the neglected segment of society during health emergencies and are left behind in global health discussions and international responses to the pandemic. Excluding refugees from national and international responses contradicts the ethics of justice that underpin public health. Actions taken to control and prevent the spread of the virus must be consistent with the international human rights norms such as non-discrimination, equal treatment, rights to health, and rights to information that apply to all persons, irrespective of their citizenship and immigration status.
Infrastructure: The pandemic has heightened the inequities within refugee communities who already reside in crowded conditions, with minimal access to water, sanitation, and hygiene (WASH) measures. Social isolation and physical distancing are practically impossible, increasing the risk of exposure to SARS-CoV-2 and forming an ideal COVID-19 breeding ground. The remote and unplanned structure of the camps offers inadequate space for creating isolation units with limited COVID-19 testing and reporting.
Health Risks: Given mental and physical traumatic experiences, refugees have greater comorbidities and underlying health conditions that make them more susceptible to COVID-19 compared to the general population. Of particular concern are high-risk groups such as the elderly, pregnant or lactating women, children, and disabled people. Lack of medical treatment to manage chronic diseases is also a factor that increases the risk of COVID-19 emergency cases among refugees.
Healthcare Services: Even before the pandemic, refugees had little access, if any, to healthcare services in the hosting country due to multiple barriers such as policy, language, and affordability. Refugees had limited access to COVID-19 testing and treatment. Refugees needing medical assistance have put even more pressure on the host country’s health care system. More importantly, vaccines, the fundamental pillar for controlling the pandemic, were not equitably accessible.
Legal Barriers: Countries require individuals to present an identification card to register for the vaccine online; many refugees are unregistered. Coupled with language-related difficulties and lack of internet access, the problem was exacerbated. Low literacy levels and limited access to reliable information have made refugees vulnerable to misinformation and promoted vaccine hesitancy. The distrust in governments, fueled by prior traumatic experiences, causes many refugees to avoid disclosing potential COVID-19 symptoms out of fear of being deported.
Economic Consequences: Pre-pandemic, some refugees worked in informal employment sectors that have been the most affected by mass layoffs. The lockdown has also left many without income if they had any at all.
Humanitarian Aid: Isolation has increased the cases of sexual and gender-based violence. Humanitarian assistance was restricted within countries as social workers had to adhere to safety precautions, lockdowns, and other governmental regulations. Additionally, funds were diverted away from refugee aid during the pandemic and fewer resources were available.
While governments continued to issue advisories, very little has been done to address the situation of refugees in the COVID-19 response.
- Advocacy: Large-scale vaccination plans should be implemented at campsites, supported by media campaigns, and in partnership with local organizations.
- Community Engagement: Accurate health-related information about the virus, preventive measures, and vaccines should be communicated to refugees in their language.
- Continuity of Services such as:
- Providing WASH services in camps
- Enabling social workers to reach the camps
- Ensuring access to COVID-19 testing
- Establishing isolation units in camps
- Providing medical support and resources (medication)
The psychosocial and health stressors have worsened the mental health state of many refugees, especially when combined with insecurity and a traumatic history of displacement, violence, and armed conflict.
One cannot ignore the fact that the negative health and economic consequences of the pandemic are immense, and recovery will be a lengthy process with uncertain timelines to overcome the pandemic. Yet, the threat of COVID-19 has no boundaries, and the current crisis demands robust action plans. Leaving no one behind is a collective, moral responsibility that has never been more urgent.
References:
- Bohnet H, Rüegger S. Refugees and Covid‐19: Beyond Health Risks to Insecurity. Swiss political science review. 2021;27(2):353-368. doi:10.1111/spsr.12466
- Ismail MB, Osman M, Rafei R, Dabboussi F, Hamze M. COVID-19 and refugee camps. Travel medicine and infectious disease. 2021;42:102083-102083. doi:10.1016/j.tmaid.2021.102083
- The Lancet. Protecting refugees during the COVID-19 pandemic. The Lancet (British edition). 2021;397(10292):2309-2309. doi:10.1016/S0140-6736(21)01366-0